What is Ewing Sarcoma?
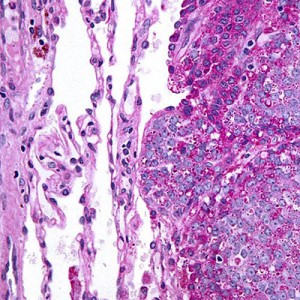
Ewing sarcoma (ES) is a malignant (cancerous) bone tumor that most often affects children. It is a rare disease in which cancer cells are found in the bone or in soft tissue. The tumor may start in the long bones of the arms and legs, the pelvis, or the chest. It may also develop in the skull or the flat bones of the trunk. The pelvis is the most common location, followed in order by the femur, tibia, humerus, and scapula. However, ES can be found in any part of the body.
Ewing sarcoma was first described by James Ewing in 1921 as a “diffuse endothelioma of bone”. He observed that this highly aggressive bone cancer was remarkably sensitive to radiation therapy.
Since the time of his description, many theories have evolved regarding how Ewing sarcomas arise. While the origin of these tumors is still not definitively known, the two theories with the most support suggest that these tumors arise from a primitive cell derived either from an embryologic tissue called the neural crest, or from resident cells in the body (called mesenchymal stem cells) that have a capability to become one of a variety of tissue types. Pathologists have long known that Ewing sarcoma looks very similar to an even rarer soft tissue tumor called primitive neuroectodermal tumor (PNET). By the early 1980’s, ES and PNET were found to not only have similar features when examined under a microscope, but in greater than 95% of cases they also had an identical genetic abnormality called a translocation. Subsequently, these two tumors have been grouped into a class of cancers entitled Ewing Sarcoma Family of Tumor (ESFT), all of which demonstrate this translocation.
What is a Translocation?
A translocation involves the mechanical breakage and reconnection between different chromosomes. Chromosomes are the cellular storage units for genes contained within the nucleus (which is the genetic center) of the cell and are analogous to a spool with the DNA or genetic message being the thread on the spool. Humans have a duplicate set of 23 chromosomes (or a total of 46 chromosomes) in any given cell that carries all of the human genes.
In ESFT, the translocation is between chromosomes 11 and 22 and is referred to as t(11;22). The gene from chromosome 22 encodes the Ewing sarcoma gene whose function is not well-understood. The gene from chromosome 11, termed FLI1, is involved in turning other genes on and off. This new fused gene, called EWS/FLI, encodes an altered fusion protein that regulates other genes that can give rise to cancers when inappropriately expressed.
Who Gets Ewing Sarcoma?
Ewing sarcoma is very rare, arising in just less than 3 per one million people under 20 years of age. In 90% of the cases, ES is found in patients between 5 and 25 years of age. It can occur any time during childhood and young adulthood, but usually develops during puberty, when bones are growing rapidly.
Boys and young men are affected more frequently than girls and young women, with a male/female ratio of 1.6:1. Males also do less well than females in terms of survival. It is 10 times as common in Caucasian children as in African-American, African, and Asian children. These ratios are consistent throughout the world.
A grouping of three unrelated teenagers in Wake Forest NC have diagnosed with Ewing sarcoma. All three children were diagnosed in 2011 and all attended the same temporary classroom together while the school underwent renovation. A fourth teenager living nearby was diagnosed in 2009. The odds of this grouping are considered significant.
Symptoms
There are few symptoms. The most common is pain and occasionally swelling at the site of the tumor.
Children may also break a bone at the site of the tumor after a seemingly minor injury (this is called a “pathologic fracture”).
Fever may also be present.
Diagnosis
If a tumor is suspected, tests to locate the primary tumor and any spread (metastasis) often include:
• Biopsy of the tumor
• Bone scan
• Chest x-ray
• CT scan of the chest
• MRI of the tumor
• X-ray of the tumor
Treatment
Ewing sarcoma is an aggressive cancer and requires 9 months to a year to treat in the best case. If the cancer doesn’t respond to “first line treatment” and if there is known disease, there are other drugs to try. If these don’t work, the patient may be a candidate for a clinical trial.
The management of ES involves physicians from multiple disciplines. It is critical that a patient diagnosed with ES is treated at a center very familiar with this disease and that the center has an interdisciplinary team of physicians and allied health care providers dedicated to this rare but deadly form of cancer. Medical specialties with expertise in Ewing sarcoma include pediatric oncology, radiation oncology, musculoskeletal radiology, and musculoskeletal pathology. Spine surgeons, vascular surgeons, and plastic surgeons may also provide critical support in some cases.
Treatment is harsh, often lasting 9 months to a year and often includes a combination of:
• Chemotherapy, including:
Cyclophosphamide
Doxorubicin
Etoposide
Ifosfamide
Vincristine
• Radiation therapy
• Surgery to remove the primary tumor
Almost all patients require multidrug chemotherapy as well as local disease control with surgery and/or radiation. An aggressive approach is necessary because almost all patients with apparently localized disease at the time of diagnosis actually have asymptomatic metastatic disease.
Currently, the treatment of all Ewing sarcoma (both soft tissue tumors and bone tumors) is the same. Based on the results of a number of clinical trials, the first line treatment is quite standardized and consists of:
• 14-17 cycles of chemotherapy, alternating between 2 regimens of drugs.
• Resection surgery if possible, which frequently involves limb-sparing surgery with prosthetic reconstruction or donor bone grafts if there is bone involvement.
• Daily radiation treatments for 6 weeks to the primary site may be required if complete surgical resection is not possible.
The tumor has a unique property of being highly sensitive to radiation, sometimes acknowledged by the phrase “melting like snow”. But the main drawback is that it recurs dramatically after some time.
Prognosis
How well a patient does depends on:
• The location of the tumor
• If the cancer has spread
The best chance for cure is with a combination of treatments that includes chemotherapy plus radiation or surgery, provided at a center that frequently treats this type of cancer.
The tumor often spreads (metastasis) to the lungs and other bones. Spread at the time of diagnosis is seen in about one-third of children with Ewing sarcoma.
Staging attempts to distinguish patients with localized from those with metastatic disease. Most commonly, metastases occur in the chest, bone and/or bone marrow. Less common sites include the central nervous system and lymph nodes.
Five-year survival for localized disease is 70% to 80% when treated with chemotherapy. Long term survival for metastatic disease may be less than 10%.
PLEASE DONATE NOW TO DEVELOP BETTER TREATMENTS FOR EWING SARCOMA
Possible Complications
The treatments needed to fight this disease have many complications, which should be discussed on an individual basis.
When to Contact a Medical Professional
Call your health care provider if your child has any of the symptoms of Ewing sarcoma. An early diagnosis can increase the possibility of a favorable outcome.
Alternative Names
Ewing’s family of tumors; Primitive neuroectodermal tumor (PNET)
The Importance of Treatment at a Specialty Center for Sarcomas
There are numerous and important reasons why someone who has been diagnosed with sarcoma should be treated at a center where there is an interdisciplinary medical team that has experience in treating this rare disease. Understandably, most patients would prefer to be treated someplace close to home, perhaps at a local oncology clinic recommended by close friends, co-workers or relatives, who had good experiences using locally available medical services. However, when it comes to the treatment of sarcomas, the advice of the experts is to take the leap and find your way to a major medical center with a specialty in treating rare, life-threatening sarcomas.
Success Rates at Sarcoma Centers
In a meticulous review of 4,205 sarcoma case records covering a 20-year period, researchers at the University of Miami School of Medicine found significantly higher success rates for patients treated at major sarcoma centers. The study entitled, “Should Soft Tissue Sarcomas Be Treated at High-volume Centers? An Analysis of 4205 Patients,” compares patient demographics; tumor type, size and location; and therapy given at low volume (LVC) and high-volume (HVC) medical facilities. Patients seen at HVC were in more critical condition than those treated at the LVC, having higher-grade tumors and correspondingly worse prognoses. Yet, patients treated at the HVC had better outcomes than their less critical counterparts treated at LVC. Patients treated at HVC were offered a broader range of treatment options, including radiation and chemotherapy in addition to surgery.
Not only did patients at HVC benefit from the use of a combination of therapies, those who had sarcomas in their extremities were also less likely to have amputations. LVC amputated 13.8% of the time, in contrast to 9.4% at HVC, where doctors have more experience with limb preservation strategies.
Fritz Eilber and Frederick Eilber of the University of California Los Angeles School of Medicine further underscore the importance of avoiding recurrence due to the use of incorrect surgical procedures. In their article “Surgical Management of Soft Tissue Tumors: Avoiding the Pitfalls,” they conclude, “The optimal treatment of locally recurrent disease is to prevent it, which necessitates aggressive surgical treatment of the primary disease, because adjuvant therapies cannot compensate for inadequate surgery.” The best way to avoid surgical errors for rare tumors (and all sarcomas are rare) is to be treated at a specialty center with an experienced multidisciplinary team.
Some Additional Considerations
In addition to the benefits of experienced medical teams, reduced surgical risk and documented lower local recurrence rates, other factors to consider in selecting a treatment center include:
• Use of precise diagnostic methods before treatment begins.
• Knowledgeable staff that will counsel patients in making decisions not directly related to their cancer treatments, such as pre-treatment fertility choices.
• Increased odds of being offered the latest, targeted therapies.
• Availability of promising clinical trials.
Patients evaluating treatment centers should also know that even the best sarcoma centers may not inform patients of, or offer to refer patients to, outside facilities for specialized services that are only available in a limited number of locations. For example, proton beam therapy, an effective treatment for some sarcomas, is only available at limited locations within the United States. A hospital that has its own IMRT (Intensity-Modulated Radiation Therapy) technology is likely to encourage patients to use IMRT rather than go elsewhere in order to receive proton beam therapy. Patients wanting to know about a wide range of treatment options should make sure they get second opinions from more than one institution and do some research ahead of time.
Patients need help finding the right place of treatment. Online sarcoma self-help and support groups are two methods that patients are using to find their way to sarcoma centers. Patients depend on the medical professionals around them to tell them the truth about their condition and what they have to do to combat it, even when it means leaving a familiar local practice for the big city hospital centers. They also need help understanding that sarcoma-related clinical trials may be the fastest route to remission.
Online Support Groups
The Online Ewing’s Sarcoma Support Group at ACOR — This group provides a network of friends who are dealing with issues related to Ewing sarcoma. An ACOR “Mailing List” is a free, non-moderated discussion mechanism for patients, caregivers, researchers, and medical professionals to exchange messages with each other. Messages are “posted” by someone on the list (i.e., a member of the support group) and cover a wide range of topics, e.g., patient experiences, research articles, clinical trials, current treatment practices and alternative treatments. A posting often results in an “online discussion” of the topic. Sometimes, one or more medical professionals are members of a support group and may comment on a posting.
Sarcoma Alliance Support Forum — The Sarcoma Alliance maintains a support forum for patients, caregivers and friends.
Planet Cancer Sarcomas Group — Planet Cancer is a community of young adults with cancer.
Connect on Facebook
The following Facebook groups provide opportunities to exchange messages with others who are dealing with ES.
• Ewing’s sarcoma
• Team Sarcoma
